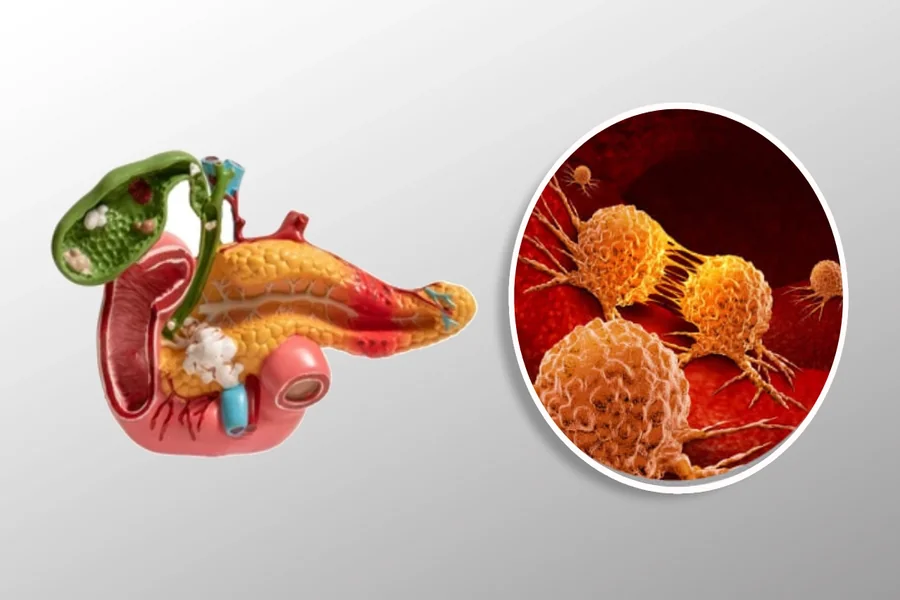
How Effective Is Pancreas Cancer Treatment? Survival Rates & Outcomes
Pancreatic cancer is often regarded as one of the more challenging cancers to treat, largely because it is frequently diagnosed at a later stage and can behave aggressively. When discussing the effectiveness of pancreas cancer treatment, it is important to recognise that success is not defined by a single outcome. For some patients, effectiveness may mean achieving remission, while for others it may involve prolonging survival or managing symptoms to maintain quality of life.
Each case is unique, and outcomes can vary significantly depending on factors such as the stage of the disease, overall health, and how the cancer responds to therapy. With ongoing advancements in medical technology and personalised care approaches, pancreas cancer treatment in Singapore continues to evolve, offering patients more options and improved outcomes than in the past.
Survival Rates: What the Numbers Really Mean
When evaluating the effectiveness of pancreas cancer treatment, one of the most referenced metrics is survival statistics, especially average 1‑year and 5‑year survival rates. In Singapore, pancreatic cancer has historically had one of the lowest survival outcomes among all cancers. According to the latest data, the overall 5‑year survival rate for pancreatic cancer patients in Singapore is about 13%, meaning roughly 13 out of every 100 people diagnosed are alive five years later. This reflects both the biology of the disease and the fact that most cases are diagnosed at an advanced stage when symptoms first appear.
It’s also important to put these numbers in context. Survival statistics are based on large groups of patients and historical outcomes, so they should be interpreted as general benchmarks rather than precise predictions for any individual. In some cases, for example, when pancreatic cancer is detected very early and is amenable to curative interventions, longer‑term survival rates can be substantially higher than the averages suggest.
The Role of Cancer Stage in Treatment Outcomes
The stage at which pancreatic cancer is diagnosed plays a critical role in determining the effectiveness of pancreas cancer treatment. Pancreatic cancer is typically classified into three main stages: localized, locally advanced, and metastatic. Patients diagnosed at the localized stage, when the tumor is confined to the pancreas, generally have the best prognosis because they may be eligible for surgical removal of the tumor, the treatment option most strongly associated with long-term survival.
For locally advanced cancer, where the tumor has spread to nearby blood vessels or tissues but not to distant organs, treatment often involves a combination of chemotherapy, radiation, and, in some cases, surgery to manage the disease and improve quality of life. In metastatic pancreatic cancer, where cancer has spread to distant organs such as the liver or lungs, the focus of treatment shifts primarily to controlling symptoms, slowing progression, and extending survival rather than achieving a cure..
Effectiveness of Surgery in Eligible Patients
Surgery remains the cornerstone of pancreas cancer treatment for patients diagnosed at an early stage. Procedures such as the Whipple procedure (pancreaticoduodenectomy) or distal pancreatectomy aim to remove the tumor entirely, offering the best chance for long-term survival. In Singapore, only about 15–20% of patients are eligible for surgical intervention at diagnosis, mainly because pancreatic cancer is often detected late.
For those who can undergo surgery, outcomes are significantly more favourable. Studies show that patients who have successful tumor removal and receive appropriate follow-up therapy can experience a 5-year survival rate of up to 20–30%, which is substantially higher than the overall average. Post-surgical care, including monitoring for recurrence and managing potential complications, is critical to maintaining these outcomes.
While surgery is not an option for most patients, it underscores the importance of early diagnosis and specialist evaluation as part of comprehensive pancreas cancer treatment in Singapore. Even in cases where surgery is possible, multidisciplinary planning with oncologists, surgeons, and supportive care teams helps optimise both survival and quality of life.
Chemotherapy and Other Non-Surgical Treatments
For many patients who are not eligible for surgery, chemotherapy, targeted therapy, and radiation therapy play a central role in pancreas cancer treatment. Chemotherapy can help shrink tumors, slow disease progression, and improve overall survival, even in advanced stages. In Singapore, common chemotherapy regimens include FOLFIRINOX and gemcitabine-based treatments, chosen based on the patient’s overall health, age, and cancer characteristics.
Radiation therapy is sometimes used in combination with chemotherapy to control tumor growth, particularly in locally advanced cases. Meanwhile, newer targeted therapies and immunotherapy are being explored in clinical trials to personalise treatment based on the genetic profile of the tumor. Although these non-surgical treatments may not always lead to a cure, they are highly effective in controlling symptoms, maintaining quality of life, and extending survival.
Factors That Influence Treatment Success
The effectiveness of pancreas cancer treatment depends on several patient-specific and disease-related factors. These can significantly impact how well a patient responds to therapy and the overall outcomes. Key factors include:
- Overall health and fitness – Patients in good general health are more likely to tolerate aggressive treatments such as surgery or combination chemotherapy.
- Tumor biology and aggressiveness – Some pancreatic cancers grow slowly and respond better to treatment, while others are more aggressive and harder to control.
- Stage at diagnosis – Early-stage cancers generally have better outcomes than advanced or metastatic disease.
- Response to treatment – Individual variations in how the cancer reacts to chemotherapy, radiation, or targeted therapy can influence success.
- Access to specialised care – Treatment at centres with experienced multidisciplinary teams, including oncologists, surgeons, dietitians, and supportive care specialists, improves both survival and quality of life.
- Personalised treatment planning – Tailoring therapy to the patient’s unique condition, overall health, and tumor characteristics optimises results.
Conclusion
Pancreatic cancer is challenging, but understanding how pancreas cancer treatment works can help patients and families make informed choices. Outcomes depend on factors like the cancer stage, overall health, and type of treatment. Surgery offers the best chance for long-term survival when possible, while chemotherapy, radiation, and newer therapies help control the disease and improve quality of life. Advances in personalised care and multidisciplinary treatment are gradually improving results.
If you or a loved one is seeking guidance, it’s important to get expert advice early. Consult our doctor to discuss your options and receive a personalised plan for pancreas cancer treatment in Singapore. Contact us at:
Dr Lee Chin Li – Lee Surgery and Endoscopy | Colorectal Surgery | Gallbladder Surgery Singapore
6 Napier Rd, #04-16 Gleneagles Medical Centre, Singapore 258499
Phone: +65 6255 0720
https://www.leesurgery.com.sg/